Definition
Epidermodysplasia verruciformis, otherwise known as, Lutz-Lewandowsky epidermodysplasia verruciformis or Lewandowsky-Lutz dysplasia is a genetic disorder of the skin that is very rare in nature. It is particularly an autosomal recessive genetic disorder, with 10 to 20% of the cases being so. Patients who inherited the disease in an autosomal recessive pattern are products of marriages that are consanguineous. Other cases, however, are sporadic, autosomal dominant and sex-linked in its fashion of transmission.
Moreover, epidermodysplasia verruciformis poses a high risk for progressing to malignant tumor or carcinoma of the skin from being a mere benign viral cutaneous lesion at the onset of the disease. The condition specifically predisposes the patient to developing cutaneous squamous cell carcinomas and multiple types of Human papillomavirus or HPV – which will more likely happen in ages 20 to 40 years old. More than 90% of patients that have epidermodysplasia verruciformis progressing to squamous cell carcinoma are infected with HPV-5 and HPV-8, respectively. Generally, the clinical course of the condition is protracted, meaning, it lasts a long time, especially longer than anyone would hope it would.
Anyhow, as an added tidbit of information, the disorder is named after the medical professionals who first detected its occurrence – Wilhelm Lutz and Felix Lewandowsky, respectively.
Epidemiology
Epidermodysplasia verruciformis has no definite age of onset; however, the condition is most commonly seen in children to young adults with ages ranging from as early as 1 year old to 20 years old. More than half of the cases onset in school age; however, there are also cases found in middle-aged people, although rare.
The progression of the benign epidermodysplasia verruciformis into malignant types may happen at the age of 40 to 50 years old, with about half of the cases actually progressing to carcinomas. The carcinoma, however, usually remains localized with a very rare occurrence of metastasis; and is limited to the skin, sparing the internal organs.
The disease has no known race partiality and no known sexual preference either.
Moreover, immunosupressed or immunocompromised hosts are very highly possible to contract the condition, as in the case of acquired epidermodysplasia verruciformis, most commonly seen in patients with lymphoma or those affected with HIV infection; and, generally in patients suffering from weakened immune system.
Causes
- As it is said, epidermodysplasia verruciformis is a hereditary or genetic disorder; hence, the etiology of the disease revolves around genetic alterations. The anomaly in the condition particularly stems out from alterations in two adjacent genes called EVER1 and EVER2, found in chromosome 17q25, as well as faulty cell-mediated immunity.
- Moving on, the products of the two genes are essential membrane proteins that are primarily linked to the endoplasmic reticulum. Two roles of the EVER1 and EVER2 genes have been cited regarding the development of epidermodysplasia verruciformis. One of which being attributed to the role of the two genes in controlling keratinocytes, which in turn plays a role in controlling HPV infection. The other role, on the other hand, is linked to the body’s immune response to the disease per se.
- However, about a quarter of the population infected with epidermodysplasia verruciformis does not show traces of alteration in the EVER1 and EVER2 genes, and their specific genetic alterations are not yet clear.
- Anyhow, another factor linked to the development of epidermodysplasia verruciformis is cases of key histocompatibility complex (MHC II) class II alleles (DR-DQ), in patients coming from regions of America, Europe and Africa. In addition, exposure to the sun in unnecessary, extended period of time may aggravate the progression of the disease.
- Lastly, although extremely rare, alterations in ras homolog gene family member H have also been cited to precipitate the development of epidermodysplasia verruciformis.
Human papillomavirus or HPV and malignant epidermodysplasia verruciformis
Cases of epidermodysplasia verruciformis are more often than not, associated with Human papillomavirus or HPV due to its high susceptibility to this kind of infection. HPV belongs to the Papovaviridae family and 30 types of which are associated with epidermodysplasia verruciformis. HPV primarily causes keratinocytic infections of the skin and are characterized as nonenveloped and predominantly minute viruses.
HPV has a lot of types that may be subdivided into highly oncogenic ones to poorly oncogenic ones. Examples of highly oncogenic HPVs are HPV types 5, 8, 10 and 47. Examples of poorly oncogenic HPVs, on the other hand, are HPV types 14, 20, 21 and 25, respectively.
The connection between human papillomavirus and malignant epidermodysplasia verruciformis principally lies on the incapability of the body’s immune system to effectively thwart off HPV infections due to a faulty cell-mediated immune response. This faulty cell-mediated immune response may be linked to an immunogenetic defect that causes the production of numerous cytokines that are highly capable of derailing cell-mediated immunity. Moreover, the T-lymphocyte production and the body’s natural cytotoxicity are significantly impaired, rendering the cell-mediated immunity incapable of fighting off HPV-infected epidermodysplasia verruciformis.
Although the types of HPV found predominatly in epidermodysplasia verruciformis patients are nonpathogenic to the general populace, these HPV types are however, significant in the condition’s progression to a full-blown carcinoma. DNAs which are viral in nature are found in these carcinomas; that, and along with other carcinogenic cofactors such as radiations from X-rays and ultraviolet rays are highly associated with cancer progression. Moreover, patients affected with epidermodysplasia verruciformis progressing to malignancies, show a low production rate of a certain genotype called interleukin 10 as compared to those who only have the benign type of epidermodysplasia verruciformis.
Furthermore, these patients affected with epidermodysplasia verruciformis progressing to malignancies show detections of E6 and E7 gene transcripts, which are mainly responsible for the HPV’s oncogenic potential. In addition, these E6 and E7 gene transcripts are highly capable of counteracting the effects of antioncogene products such as p53 and pRb, respectively. Lastly, E6 and E7 have the capacity to promote cell growth that may precipitate the formation of malignancies.
The combination of HPV types, which are higly oncogenic such as HPV, types 5 and 8, and these E6 and E7 viral genomes coupled with a malfunction in programmed cell death to eradicate damaged DNAs, are highly linked as the main causative factor for the progression of a benign epidermodysplasia verruciformis into malignant ones.
Signs and Symptoms
- Epidermodysplasia verruciformis is usually typified by a constant, persistent infection with Human papillomavirus or HPV. Common signs and symptoms are partial to integumentary manifestations with a very rare mucosal incidence. Frequent integumentary manifestations are lesions that resemble the appearance of warts, extensive skin outbreak that are even to papillomatous in nature and reddish to brownish pigmented plaques located in various parts of the body such as the hands, forearms, legs, trunk and the face.
- There are cases where epidermodysplasia verruciformis is isolated or localized in one area and has persistent occuring warts that are papule-like in appearance. Furthermore, this case has characteristics that very much resemble that of psoriasis.
- Other cases of epidermodysplasia verruciformis, on the other hand, are predominantly spots that are white in color and very much resembles tinea and pityriasis versicolor, which usually develops in the trunk area. Pityriasis versicolor, by the way, is a pale, rash caused by a yeast-like germ.
- Chronologically, however, the condition appears flat, wart-like lesions in the early stage of life such as in infancy and childhood. Moreover, the plaques usually join together to form one united plaque in the upper extremities, neck and face.
Epidermodysplasia Verruciformis Pictures
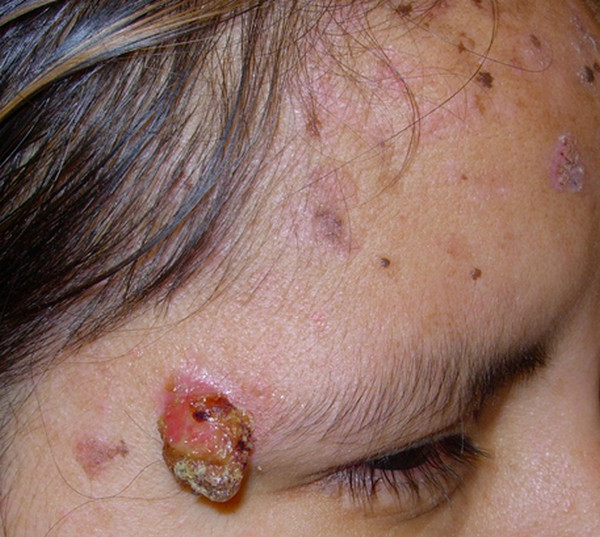
Picture 1 : Epidermodysplasia Verruciformis (on head)
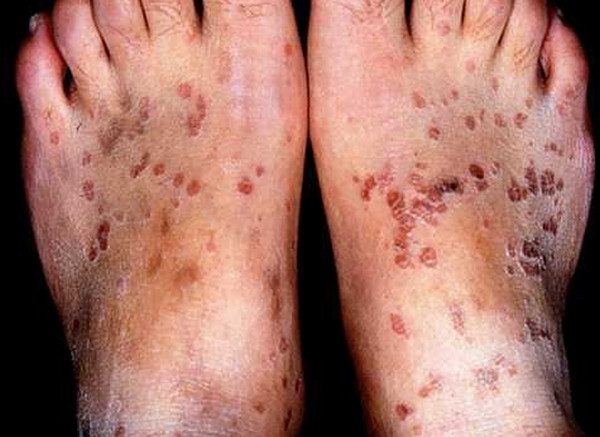
Picture 2 : Epidermodysplasia Verruciformis (on feet)
Types of Epidermodysplasia Verruciformis Lesions
Although epidermodysplasia verruciformis may present in several forms (polymorphic), two characteristic types were cited, which are the flat types and seborrheic-like or verrucous types, respectively.
The first type is as mentioned, flat or even lesion with flat-topped papules, resembling a wart and verruca plana with scaly surfaces and either hypopigmented or hyperpigmented patches. Moreover, small patches may fuse or come together to form prominent, large patches with irregular borders. In addition, the patches may vary from reddish to brownish in color and is usually persistent.
The seborrheic-like or verrucous type, on the other hand, is prominently presented as resembling the appearance of a wart. The lesions usually form a linear column in areas of the body that are exposed to the sun, such as the upper and lower extremities, neck, face (usually in the forehead area) and even the earlobes; although, the lesions may also appear in areas like the soles of the feet, the genital area as well as the axillae or the underarm area. Infrequent locations are the moist parts of the body such as the oral mucosa and conjunctivae. The patches in this kind of epidermodysplasia verruciform are slightly elevated and brownish in color.
Differential Diagnosis and Tests
The diagnosis of epidermodysplasia verruciformis should be initiated upon the appearance of verrucous (rough, wart-like) lesions and when the condition is not relieved by the administration of a treatment regimen.
A highly competent medical professional does the diagnosis and laboratory studies are usually performed to detect HPVs, usually through in situ hybridization. Conformational polymorphism analysis may also be performed to detect specific EVER1 and EVER2 gene alterations. The faulty cell-mediated immunity may also be identified by employing various laboratory methods.
As in most cases, a biopsy may be also performed by medical professionals to aid in correctly diagnosing the disorder. The primary purpose of the biopsy however, is to work up precarcinoma and malignant lesions, as well as identify HPV-related epidermodysplasia verruciformis.
Differential diagnosis should also be done in order to rule out other disorders such as tinea versicolor, squamous cell carcinoma and warts.
Treatment
There are various therapeutic regimens that the health provider may opt for the treatment of epidermodysplasia verruciformis; such therapeutic regimens are as follows:
Pharmacologic Therapy
Examples of medications administered to treat or perhaps, alleviate the effect of the condition are systemic retinoids (acitretin and isotretinoin), topical 5-fluorouracil and imiquimod, respectively. Moreover, the administration of interferon, in adjunct with retinoids has also been utilized. Photodynamic therapy has also been cited as an effective treatment method for epidermodysplasia verruciformis.
In cases of HPV-linked epidermodysplasia verruciformis, an experiment regarding the use of a mixture of cholecalciferol (Vitamin D) or interferon alpha analogues and 13-cis retinoic acid as a pharmacologic treatment is also underway.
Surgical Intervention
The surgical intervention that may be performed for isolated carcinomas is the autotransplantation of skin from unaffectected areas. This method has shown promising results in prevention of further carcinomas.
In addition, employment of cryoprobes to remove benign lesions on the skin, as well as grafting of the skin from areas of lesser or no exposure to the sun, may also be utilized.
However, if the epidermodysplasia verruciformis has already progressed into a carcinoma that is invasive in nature, then a surgical excision may be necessary to prevent further problems.
Supportive Care and/or Preventive approach
However, generally, the medical management of epidermodysplasia verruciformis does not guarantee full resolution of the disorder, as one lesion removed may only recur along the course of the patient’s life. That is why, more often than not, the medical management of the condition is primarily directed to a preventive approach such as avoidance of oncogenic factors, like UV lights A and B; and X-ray radiation among others.
In addition, the health care provider should also provide patient counselling and education, and counselling to the patient’s significant others as well. The patient, together with his/her significant others in return, should be vigilant about heeding these preventive factors discussed in the counselling. The use of sun block or sun protection may also be necessary as a defense from the sun’s harmful UV rays.
Assistance to the patient in maintaining good hygiene should also be provided. In addition, a balanced healthy diet coupled with fresh fruits and vegetables should also be observed, as this may be beneficial to the patient’s skin health, as well as overall health.
Prognosis
Epidermodysplasia verruciformis progresses throughout the course of a patient’s life and may ultimately lead to the development of carcinomas. However, as stated above, metastasis rarely occurs. Furthermore, mortality rate may be significantly reduced if the condition is detected at an early stage and the appropriate treatment therapies are employed properly.
References
http://emedicine.medscape.com/
http://en.wikipedia.org/wiki/