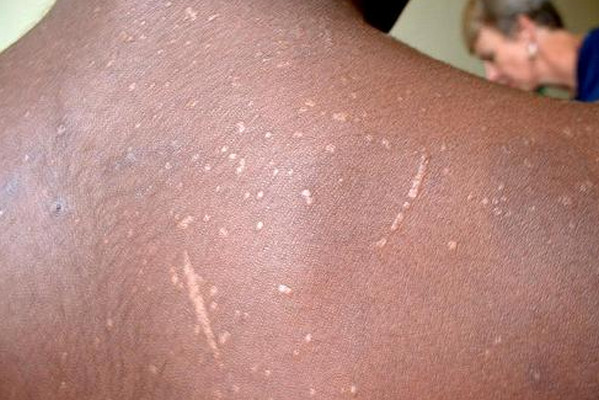
What is HIV Rash?
HIV rash is a symptom of Human Immunodeficiency Virus or HIV that commonly appears at the 2nd or 3rd week of the course of the disease. HIV rash may be considered as a warning sign that an infection is already present in the body. It is usually located in the central part of the body, anterior and posterior trunk and around the face and the neck up to the limbs and hands. In addition, an estimate of 85% of HIV infected patients will develop HIV rash.
However, not all presentations of a skin rash translate to an HIV rash. Due to some similarities of an HIV rash to those rashes that occur in other skin conditions and allergic reactions, it is important to consult a physician before assuming anything to prevent confusion and unnecessary hassle.
Pathophysiology of HIV Rash
Since HIV rash is a symptom of an infectious disease called Human Immunodeficiency Virus or HIV, understanding how HIV rash occurs includes knowing the pathophysiology of HIV.
Infection Stage
HIV is an infectious disease. The ability of the body to resist infection, or immunity, is the first line of defense. HIV is an intracellular parasite called retrovirus. Instead of the common phenomenon of the genetic material being carried off in an organism’s deoxyribonucleic acid or DNA, the genetic material in a retrovirus is contained in its ribonucleic acid or RNA.
These viral RNA is encased, and this case comes with a glycoprotein that is usually sticking out of the envelope. This glycoprotein is the one mainly responsible for enabling the HIV to enter its goal cell. For the “invasion” to be successful, the viral envelope should be able to fuse to the goal cell’s plasma membrane.
Primary Infection stage
The primary infection stage is usually when HIV rash appears. It is the stage or period from the time infection occurs up to the time where antibodies are developed to fight off HIV. This is the period where intense proliferation of the virus occurs, as well as its widespread dissemination throughout the body. At this early part of the primary infection stage, the person may experience no symptoms at all or severe flu-like symptoms.
However, in the 3rd week, the person starts to manifest signs and symptoms, especially HIV rash. Most of these symptoms resemble those of mononucleosis’ symptoms. Aside from HIV rash, the person may also have:
- Muscle aches,
- Headaches
- Enlarged lymph nodes
- Fever
- Joint pain
- Diarrhea
- Sore throat
- Mouth or genital ulcers and/or
- Night sweats. [3]
Viral Set Point
This is the stage where the antibodies that fight off HIV (immune response) are roughly the same amount as those of the number of HIV in the body. This means that the individual is, at this time, in a steady state of infection. This viral set point may last for a few years.
HIV Rash Causes
HIV rash may have its origins as a viral, or bacterial or fungal infection, or as a drug reaction. That is why it is essential to seek medical attention promptly for proper diagnosis and treatment. [4]
HIV rash can occur at any stage throughout the course of HIV infection. In the acute or initial stage of infection, the HIV rash appears as a generalized condition, which means it looks like a “common” rash. Consequently, it is usually mistaken as something else, such as an allergic infection. This occurs at around 2nd to 3rd week of the disease.
In the chronic stage of the disease however, the HIV rash may appear as a symptom of various integumentary infections. One of these associated integumentary infections is seborrheic dermatitis. Seborrheic dermatitis is one of the most common integumentary manifestations of the HIV disease. The HIV rash in seborrheic dermatitis is usually scaly or flaky in nature, indurated and diffused throughout the face, scalp, chest and even the groin area.
Another integumentary infection in the chronic stage which appears as an HIV rash is the herpes virus infection. The HIV rash from herpes infection is reddish in color and typified with blisters that are characteristically fluid-filled. In addition, there is also an HIV rash, caused by an HIV complication called Drug Rash with Eosinophilia and System Symptoms or DRESS. This HIV complication appears as a characteristic HIV rash of its own and usually requires immediate medical attention.
Another cause of HIV rash is drug-related. This usually happens when there is an adjustment of dosage of the current medication or if the HIV physician has decided to switch to another medication. In these cases, there is a high possibility of resulting skin irritations. This resulting HIV rash usually resolves as the patient gets used to the adjustment of dosage or to the new medication. However, if the HIV rash does not go away naturally, consult the HIV physician about it.
More than half of the individuals treated with trimethoprim-sulfamethoxazole (TMP-SMZ) develop this drug-related HIV rash. This HIV rash is itchy or pruritic in nature and is accompanied by the presence of pinkish-red macules and papules.
All of these HIV rashes are all sources of discomfort to the patient. In addition these rashes result in a higher rate of infection because the integrity of the skin has been compromised.
Characteristics of HIV Rash
Different opportunistic infections may present different HIV rash appearances. The shape and size of HIV rash may vary. Some may present as only little dots while others may appear in large clusters throughout the body. The most common characteristic of an HIV rash is that one of purplish to blackish in color for dark-skinned individuals, and reddish to brownish in color for light-skinned individuals. Also, it is usually similar to an eczema, because it may present as a reddish to brownish razor skin bump.
The HIV rash may also be pruritic in nature. Also, HIV rash may be accompanied by fever, fatigue, white patches in the mouth or oral thrush, loss of appetite, loose bowel movement and resulting loss in weight. Blisters may also appear in the body’s mucous membranes such as the mouth, eyes or the genital area. Peeling of the skin may also occur. Extreme complications of HIV rash may include problems involving vision and loss of memory.
HIV Rash Pictures
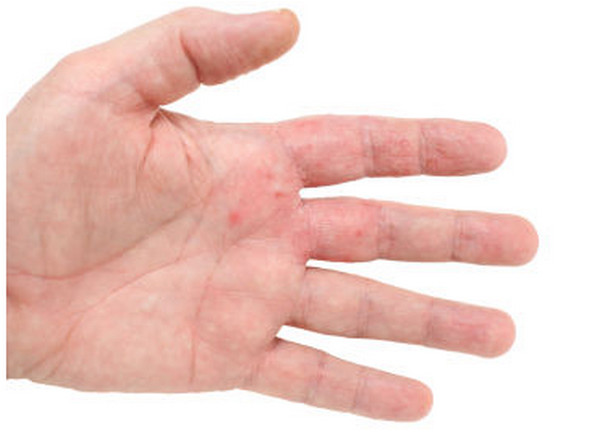
Picture 1 : HIV Rashes on hands and fingers
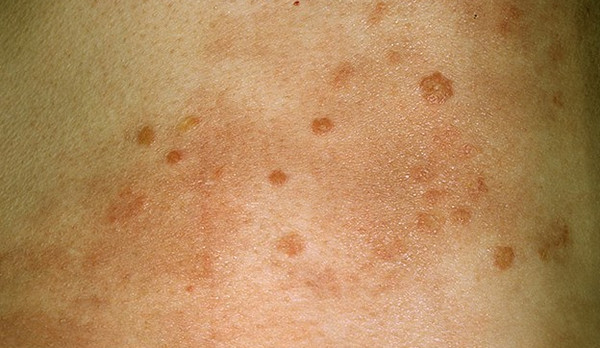
Picture 2 : HIV Rashes on all over body
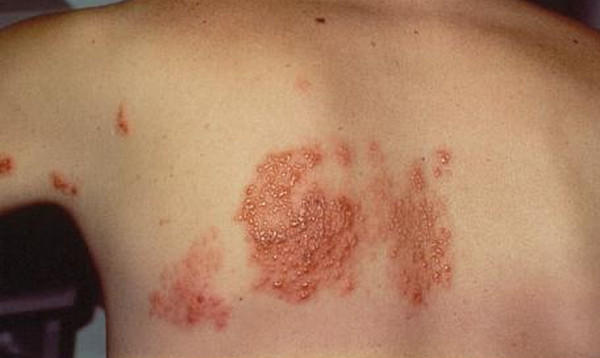
Picture 3 : HIV rashes (red) on back
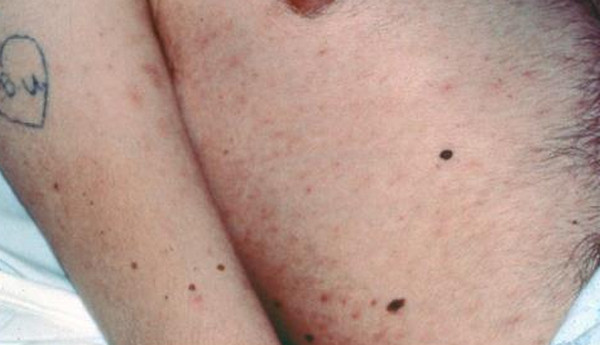
Picture 4 : HIV Rashes on chest and trunk
Picture 5 : HIV Rashes on shoulders
Medical Management of HIV Rash
If a person develops an HIV rash, it is very important not to self medicate. Self-medication may only worsen things. Consult with an HIV physician. This HIV physician will determine the cause and nature of the HIV rash, as these rashes occur with various underlying conditions. When the correct cause is determined, then the appropriate treatment will then be employed.
Pharmacologic Therapy
To control pruritus or itching and the swelling of the HIV rash, over the counter drugs are usually administered to control it. Example of these over the counter drugs is Benadryl, a hydrocortisone cream. Moreover, if the underlying condition related to the HIV rash is already severe in nature and the resulting pain is already debilitating to the patient, then the HIV physician may administer analgesics as needed or at regular intervals, around the clock.
Alternative Treatment Regimen
Exposure to extreme temperatures, whether be it extreme heat or extreme cold may aggravate the HIV rash. Therefore, the HIV physician may advise the patient to avoid hot bath and showers, direct sunlight and extremely cold environments. [5]
Also, be vigilant about the food and medicine intakes, and even soaps and other skin products that have come in contact with the skin prior to the appearance of HIV rashes, as these HIV rashes may be caused by an allergic reaction to these things.
Some nutritional supplements may be helpful to minimize specific symptoms, such as fish oil or whey protein. Others can be detrimental such as St. John’s Wort or garlic supplements. [3]
Furthermore, if a patient is advised to stop taking a certain medication due to the appearance of an HIV rash, do not restart it when the rash symptoms are relieved. Never do things in your own way. Always consult the HIV physician before taking any action regarding treatment regimen.
Practice proper hygiene. Rashes can occur due to irritation from dusts and even unwashed, dirty clothes. By practicing proper hygiene, the patient can avoid HIV rashes which are associated with personal sanitation.
Avoid unprotected sexual activity. Tight fitting clothing and harsh chemical soaps can also irritate the skin and make it more vulnerable to HIV rash.[6]
Supportive Therapy for HIV Rash
Severe skin breakdown may be very debilitating to the patient. Hence, supportive care is necessary to be provided to the patient. Supportive care includes assisting the patient in meticulous and thorough skin care. Moreover, the patient should be turned regularly (preferably every two hours) to prevent bedsores and further damage to the weight bearing skin affected by the HIV rash. Assistance with applying topical medications and dressing should also be provided if necessary.
Pain associated with HIV rash may also be relieved or alleviated with the use of relaxation techniques such as deep breathing exercises (if the patient is able to do so), as well as guided imagery.
References:
- http://www.livestrong.com/
article/154733-early-symptoms- of-the-hiv-virus/ - http://www.health.com/health/
gallery/0,,20539037_6,00.html - http://www.mayoclinic.com/health/hiv-aids/DS00005/METHOD=print
- http://symptomstreatment.org/hiv-rash/
- HIV rash
- http://www.hivsymptomsonline.com/hiv-rashes.html
- http://emedicalhub.com/hiv-rash-symptoms-pics-treatment/